Reproductive effects of antiepileptic drugs
Reproductive effects of antiepileptic drugs
Effect on hormones
A large number of epileptic patients are treated with more than one antiepileptic drug at a time. Many of the studies assessing the influence of medication have not been able to correlate effects with specific drugs or, if they have, only a few patients have been available for investigation. Results are sometimes variable between different studies but the following changes appear to be the most consistent. 
Sex hormone-binding globulin (SHBG) levels are increased, which leads to a reduction in the level of free testosterone. Total testosterone levels (which includes both free hormone and that bound to proteins such as SHBG) are either normal or elevated. LH levels are usually significantly increased. Toone and co-workers were able to correlate the reduction in free testosterone level to two aspects of sexual drive, namely the frequency of early morning erections and sexual activity leading to orgasm.
There are two explanations for the hormone abnormalities seen. One possibility is that antiepileptic drugs induce liver enzymes thereby increasing the production of SHBG. This binds more testosterone, reducing the amount of biologically active free testosterone. Pituitary LH is secreted in greater amounts to try to increase testicular testosterone production. Alternatively, it is possible that the primary abnormality is a reduction in free testosterone as a consequence of increased metabolism. This leads to a rise in LH to increase testosterone synthesis, accompanied by a secondary rise in SHBG.
Macphee et at noted that untreated epileptics had hormone levels similar to healthy controls. They investigated hormone concentrations in epileptics taking carbamazepine, phenytoin and sodium valproate as well as patients taking multiple drug combinations. Patients on multiple drugs had abnormalities of all hormones measured, including raised
SHBG, reduced free testosterone and high LH levels. In contrast, drugs used individually only appeared to have isolated actions. For example, carbamazepine was associated with reduced free testosterone levels and high LH but normal SHBG. Phenytoin, however, caused a significant increase in SHBG levels without a significant effect on free testosterone. It should be noted that in three of the thirteen patients on phenytoin, free testosterone levels were below the lowest of the 40 control patients. Sodium valproate had no effect on any of the hormones measured. It follows that different antiepileptic drugs exert their effects via different mechanisms.
Carbamazepine had no effect on SHBG levels; therefore, it probably reduces testosterone by increased hepatic clearance of testosterone. For phenytoin, increased SHBG synthesis may be the more important mechanism. This study did demonstrate that sodium valproate may be a good alternative treatment for male epileptic patients with sexual dysfunction. Whether these hormone changes are sufficient to explain the reduced sexual function in epileptic patients is uncertain. For example, in one study in men, decreased libido and potency were more often reported with use of phenobarbitone or primidone than with phenytoin or carbamazepine, despite the fact that all four drugs are potent inducers of liver enzymes.
Less information is available on the effect of epilepsy on female reproductive function. It is recognised that in some women the frequency of epileptic seizures is higher in the late follicular phase when oestrogen levels are high and reduced in the mid-luteal phase when progesterone levels are maximal. There have been some studies which suggest that women with epilepsy are more likely to have irregular menstrual cycles linked to anovulation, but gonadotrophin levels were not measured to assess if this was an ovarian or hypothalamic-pituitary effect. The fertility of epileptic women has not been directly studied.
Effect on sperm
Epileptic patients often receive long-term medication and combined antiepileptics. Toone and co-workers suggested that long-term treatment may lead to testicular failure and impaired spermatogenesis. Alterations to sperm parameters, including motility, were first described in 1975, but only a few studies have tried to investigate this in more detail. It has been suggested that as antiepileptic drugs suppress neuronal irritability by stabilising cell membranes they may also have an adverse effect on sperm membranes. One study assessed sperm parameters in a group of 10 epileptics receiving long-term medication. 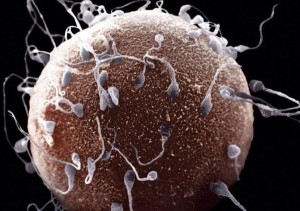
Five were taking phenytoin alone and the others were receiving multiple therapy. Sperm motility was quantified by assessing the ability of the sperm to migrate across a micropore membrane. Motility measured in this way was significantly reduced in the treated epileptic patients compared with healthy donors. The authors also performed an in vitro study in which the motility of donor sperm was assessed after addition of high concentrations of antiepileptic drugs to the sperm preparation. The drugs did adversely affect sperm motility in vitro but only at concentrations much higher than those found in the clinical context. The authors noted that they were only looking at acute exposure, whereas treated epileptics are chronically exposed to these drugs.
A recent study has looked at conventional sperm parameters in untreated epileptics, epileptics treated with long-term phenytoin and healthy controls. Interestingly, semen volume was reduced in both treated and untreated epileptic patients. Both these groups also showed significant reductions in sperm concentration compared with controls. There was no difference between treated and untreated epileptic patients.
These results raise the possibility that fertility may be reduced in epileptic patients irrespective of treatment, although there is no direct evidence for this in the literature. It has been suggested that the apparent reduction of fertility in epileptic men may be related to hyposexuality and the absence of a sexual partner.



















